HEALTHCARE ECONOMICS
The healthcare sector – private and public – relies on the monetary value of the system, even if its goal is ideally related to helping people live healthier lives rather than generating profit. In most countries, the health sector is a multi-billion dollar industry. The World Health Organization estimates the global health industry spent over $8 trillion in the year 2018. We previously explored some of the adverse health implications associated with low health literacy; however, it is also imperative to discuss the financial impact of low health literacy.

THE COSTS OF LOW HEALTH LITERACY
Based on a 2015 study published in the International Journal of Health Policy Management, people with low health literacy contribute to more costs and use health services more often than those with proficient health literacy. In a 2017 cross-sectional analysis, researchers found that patients with low health literacy are at greater risk for adverse outcomes such as medication errors, hospital readmissions, and death.
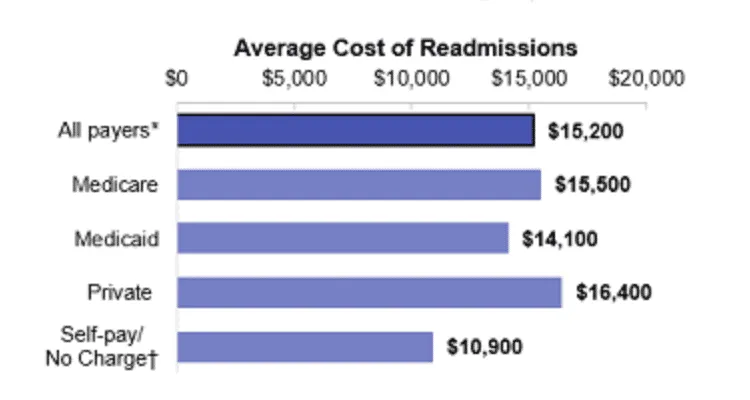
Hospital readmissions comprise a critical health issue and account for a significant percentage of overall expenditures. Researchers examined the average costs of hospital readmissions within 30 days; their results indicated the average hospital readmission cost per payer is approximately $15,000 (shown in the graph below).
Even more telling of the 30-day hospital readmissions, Medicare- and Medicaid-holding patients accounted for the majority of those readmitted within 30 days. In the year 2018, the total number of adult hospital readmissions within 30 days was 3.8 million. This further reveals the extent of hospital readmissions regarding overall healthcare spending.
According to a 2007 meta-analysis conducted by the University of Connecticut, low health literacy costs the United States economy up to $236 billion annually. By working to improve health literacy rates over time, the U.S. economy alone can save nearly $1.6 trillion. Their findings recommend two policy interventions: 1) increasing the number of those with health insurance coverage and 2) most importantly, improving how health providers relate to and exchange information with patients.
HEALTH POLICY INTERVENTIONS
The interactions between health providers and patients reveal crucial information. To improve communication, access to digital patient education materials seems most promising. Digital patient education materials aid in the accessibility of health information since they rely on the far-reaching nature of digital technology. Some types of digital health technology include telemedicine, wearable devices, and mobile health. In sum, digital technology is not dependent on location or time.
The effects of digital health education technology show improved learning, especially for those with low health literacy. Researchers from a 2018 review study found low health literacy patients who received spoken animation and illustrated text showed improved recall. Thus, digital technology may be an effective tool to teach patients complex information.
The prevalence of low health literacy in a population not only affects the health of an individual but places a significant financial strain on a country’s economy. Addressing low health literacy has great potential to unburden taxpayers and private payers alike. Digital health interventions to improve health literacy should use a universal approach that optimizes educational resources, especially directed to the most vulnerable population groups.